Predicting needs to target care
Is it possible to use data modelling to leverage the data collected by community health workers and predict households likely to need urgent care? Living Goods is doing it and it works.
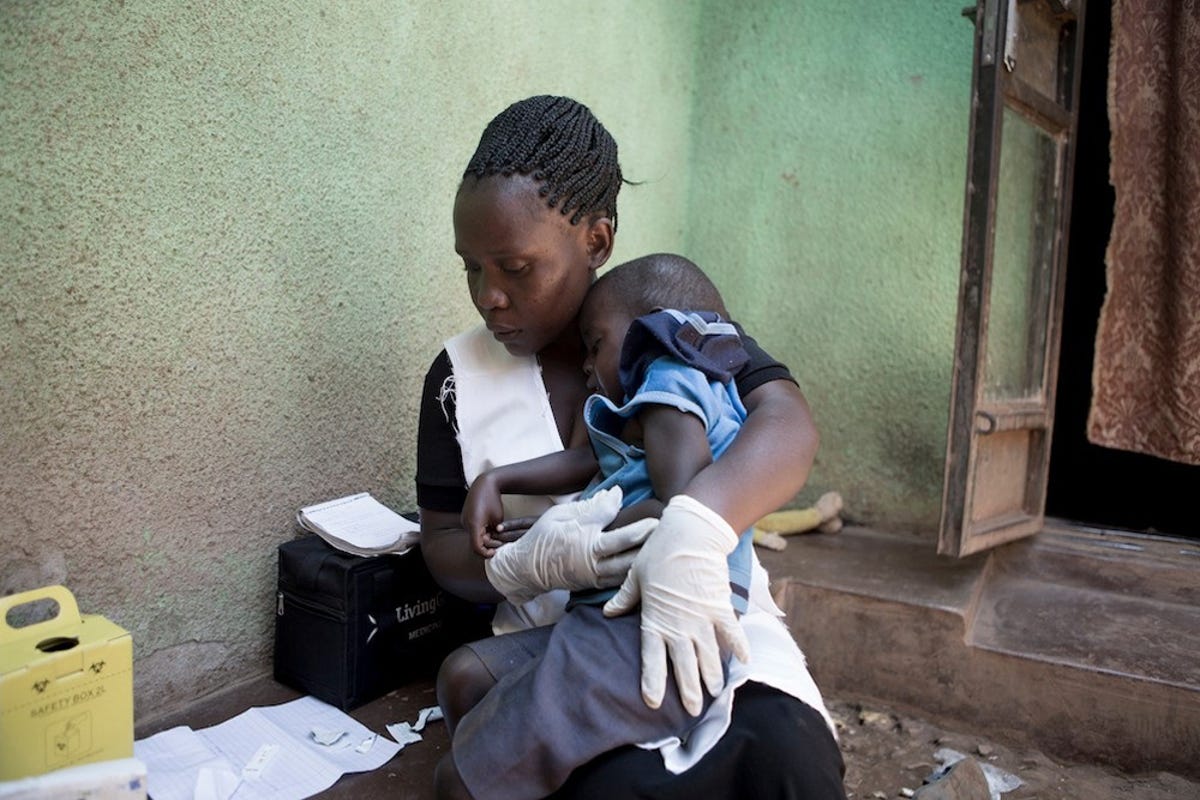
© Living Goods / Georgina Goodwin
We usually imagine a doctor’s office or hospital when we think of healthcare. But in most rural areas of the world, Community Health Workers (CHW) are the first line of medical help.
CHWs are key members of the communities they live in and serve, who share the language, culture and connections of their neighbours and thus provide a critical link between their communities and the primary healthcare system.
In Africa, with variations from country to country, they provide primary healthcare support which can extend from counselling and referrals to the treatment of adult non-communicable diseases and maternal and paediatric healthcare. Sometimes, but not always, they deliver family planning education and medicines, and drive demand for essential immunisation services. Now early detection of COVID-19 is often also their responsibility.
In Kenya and Uganda, Living Goods – a non-profit dedicated to building sustainable community health systems at scale – supports networks of government CHWs to ensure these front-line workers are digitally-enabled, properly equipped, effectively supervised and fairly compensated so they can deliver high-level community health services door-to-door.
Today this network includes nearly 8,500 government CHWs in Uganda (including CHWs supported by partner BRAC Uganda,) and more than 3,090 in Kenya, who are collectively providing community health coverage for over 8.5 million people.
With an effective network of CHWs in place, Living Goods’ challenge soon became how to measure and maximise the efficiency and equity of its health service delivery. While still used for educating community members, paper flipbooks proved cumbersome for diagnostic note-taking and data collection and made standardisation and continuity of care difficult, slow and unreliable. There was a clear need to improve the CHW workflows to better support their invaluable contributions to community health.
Partnering with – a non-profit focused on building open-source technologies that support CHWs in their work – Living Goods co-designed a mobile app called the Health App to enable real-time on-site data collection, improve and automate diagnosis and follow-up, and drive improvements in performance management. The Smart Health App digitally captures a mobile number and GPS location for every patient visit, provides supervisors with dashboards that help them monitor the performance of every health worker and enables CHWs to optimise their time with those patients at highest risk, because it provides them with daily task lists and reminders.

© Living Goods / Martina Bacigalupo
But efficacy was not Living Goods’ and Medic’s only objective: they also wanted to understand at a more granular level if the CHWs they support were reaching the households most in need of assistance in each community. Measuring the equity of healthcare delivery was a key priority. For this, they incorporated an tool in the App to provide a simple, free and accurate way of measuring and categorising households based on wealth and national benchmark data.
The Smart Health App has been in use since 2015 and constantly improved over time to better impact key health metrics and identify the populations in most need. Living Goods has built up its internal tech team and now develops many workflows independently.
In addition, Living Goods and Medic piloted predictive algorithms to leverage the large amount of data collected by the CHWs using the App, including more recent data on immunisation and family planning. These algorithms use data modelling to identify households with expectant mothers less likely to deliver at a health facility and new-borns and children under the age of 5 with a danger sign and possibility of not being visited by a CHW on time.
“We used various indicators, such as wealth quintile, location of household in relation to health facility, danger signs identified during pregnancy and number of children, to predict households likely to need urgent care,” explained Andrew Karlyn, Living Goods’ Chief Impact Officer. “This allowed us to narrow the original risk factors identified down to three: the probability of a child getting sick and being tended to within 72 hours, the probability of facility delivery and the probability of a newborn developing danger signs. Our aim was to predict which children are most likely to get sick and to help flag these cases to CHWs so they can proactively visit and check in.
“For pregnancy-related risks, our aim was to predict which women were unlikely to deliver in a health facility, as well as which women were most likely to deliver babies with a high probability of developing danger signs. We developed models for each of these three use cases.”
The pilot ended in November 2019 with significant insights on how best to run a predictive model and led to a number of flagged cases. Living Goods is now looking to enhance these learnings with other researchers to explore the feasibility of leveraging data and the insights gathered for predicting immunisation default.